Translate this page into:
Epidermal inclusion cyst after uneventful small incision cataract surgery: A diagnostic dilemma
-
Received: ,
Accepted: ,
How to cite this article: Kaur R, Dahiya P, Rai S, Roychoudhury AK. Epidermal inclusion cyst after uneventful small incision cataract surgery: A diagnostic dilemma. Glob J Cataract Surg Res Ophthalmol. 2023;2:69-72. doi: 10.25259/GJCSRO_24_2023
Abstract
Conjunctival cysts are not so uncommon after surgical procedures. They are usually benign in nature and are filled with serous material and mucous. They may be congenital or acquired in origin. Acquired cysts are mostly seen after ocular surgery and trauma. Hereby, we report two cases of conjunctival inclusion cysts following uneventful manual small incision cataract surgery in two elderly females. Both cases were treated by cyst excision and suturing of the scleral tunnel with interrupted sutures was done. An unstable scleral wound may be a contributory factor in the formation of cysts. Hence, we conclude that closure of the scleral tunnel with overlying tenon and conjunctival apposition is a critical step in controlling such complications of cataract surgery.
Keywords
Epidermal inclusion cyst
Small incision cataract surgery
Uneventful
INTRODUCTION
Conjunctival inclusion cysts are benign cysts. They are clear and transilluminating when filled with serous fluid only. Histologically, they are characterized by a lining of stratified squamous nonkeratinizing epithelium. These cysts are filled with serous fluid and shed cells. Conjunctival inclusion cysts can be categorized as either congenital or acquired, with the latter being associated with trauma or surgical interventions.[1] While acquired conjunctival inclusion cysts are frequently observed following strabismus surgery,[2] they can also manifest after other ophthalmic procedures, including pars plana vitrectomy,[3] scleral buckling,[4] ptosis surgery[5] and Ahmed glaucoma valve insertion.[6] Interestingly, while there have been reported cases of conjunctival inclusion cysts following phacoemulsification surgery, there are few documented instances following manual small incision cataract surgery (SICS).[7,8] The incidence rate from the previous reports on unintended filtering blebs after cataract surgery varied between 1% and 7.7%.[9,10]
Recently, we encountered two cases where patients expressed significant anxiety concerning the presence of painless swelling following uneventful SICS.
CASE SERIES
Case 1
A 67-year-old female presented with a complaint of foreign body sensation and swelling in her left eye that had been persisting for 10 days. The cystic swelling was painless and firm non-mobile which had gradually increased in size. The patient had previously undergone a SICS with posterior chamber intraocular lens (PCIOL) implantation in her left eye 20 days back. On examination of both eyes, the best-corrected visual acuity (BCVA) was measured as 20/60 in the right eye and 20/40 in the left eye. Corrected goldmann applanation tonometry (GAT) was 16 and 12 mm Hg in the right and left eye, respectively. The anterior and posterior segment evaluation was unremarkable, except an isolated cystic non-mobile swelling was observed at the superior limbus in the left eye, directly over the previous scleral tunnel. The swelling measured 6 × 8 mm and contained clear fluid. The transillumination test was positive. It looked like a tunnel freely communicated with the cyst. Seidel’s test was negative. The patient was scheduled for surgical excision of the cyst under local anaesthesia. Intraoperatively, the conjunctiva surrounding the cyst was separated through gentle dissection, and during the excision process, the cyst ruptured from its base with the release of clear fluid. The cyst was found to be entrapped in the SICS tunnel resulting in the fish mouthing of the tunnel. However, it was not found to be freely communicating with the anterior chamber. A part of the excised cyst was sent for histopathological examination. Three 10-0 interrupted sutures were placed on the scleral tunnel for watertight closure followed by re-approximation of the conjunctiva. The underlying sclera was cauterized, and the conjunctiva was re-approximated to the limbus. Postoperatively, an antibiotic and steroid combination was started. Histopathological examination revealed an epidermal inclusion cyst. On the postoperative day 1, there was mild congestion with one knot protruding out with a well-apposed tunnel with the stability of vision and normal intraocular pressure [Figures 1a-c].
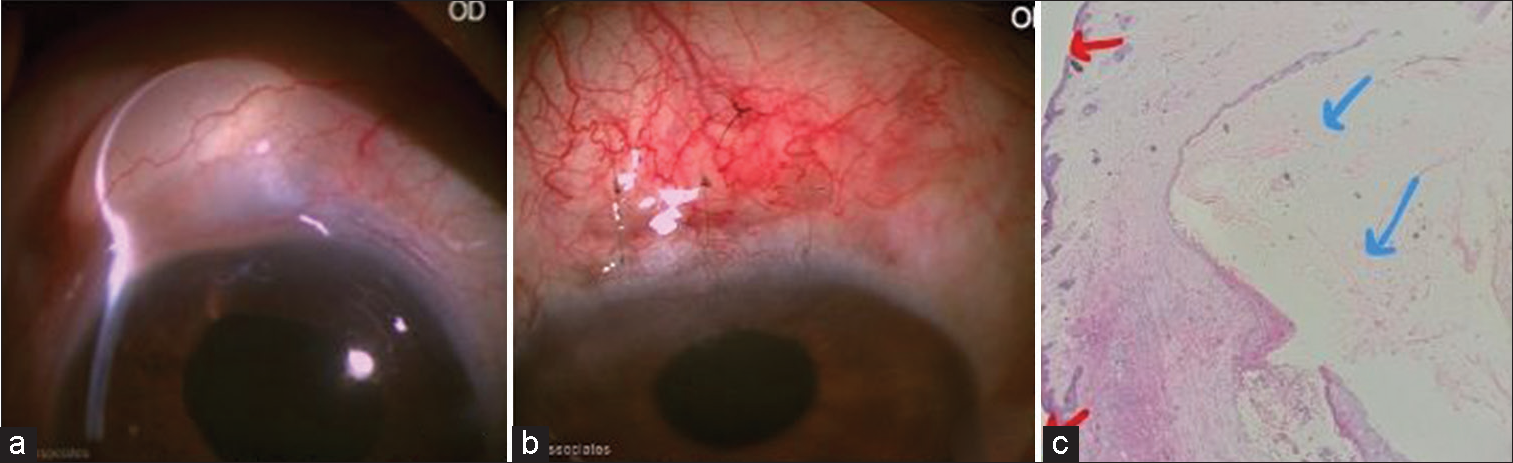
- Case 1: (a) Before excision cystic swelling on transillumination test. (b) One first day post-operative. (c) Histopathology picture showing keratinised stratified lining epithelium (red arrows), and keratin flakes (blue arrows).
Case 2
A 78-year-old woman presented with a persistent swelling and foreign body sensation in her right eye, which had been bothering her for the last 25 days. The swelling was painless and had gradually increased in size. Approximately 1 month ago, the patient had undergone SICS with the implantation of a PCIOL in her right eye. During the examination of both eyes, the BCVA was measured as 20/60 in the right eye and 20/40 in the left eye. The intraocular pressure was 14 mmHg and 16 mmHg in the right and left eyes, respectively, measured by GAT. A distinct cystic swelling was observed at the superior limbus in the right eye, directly over the previous scleral tunnel incision. The swelling measured 3 × 6 mm and contained mucinous fluid. Seidel’s test was negative. Dilated fundus examinations were unremarkable with no signs of hypotony. The patient was scheduled for surgical excision of the cyst under local anaesthesia. Intraoperatively, the conjunctiva surrounding the cyst was delicately separated, inadvertently leading to the rupture of the cyst from its base during the excision process. The cyst was found to be communicating with the scleral tunnel. It ruptured while excising, and a part of it was sent for histopathological examination. The underlying sclera was cauterized and the scleral tunnel was sutured with three interrupted sutures and the conjunctiva was carefully re-approximated to the limbus. Histopathological examination revealed a cyst lined by keratinised stratified squamous epithelium. The postoperative period was unremarkable, the wound was well sealed, and improvement in the BCVA to 20/20 and normal intraocular pressure [Figures 2a-c].

- Case 2: (a) Before excision with seromucinous fluid. (b) Post-operative (15 days). (c) Histopathology shows a cyst lined by keratinised stratified squamous epithelium. The wall of the cyst was lined by fibrous tissue with few inflammatory cells (yellow arrow). The lumen of the cyst showed numerous keratin flakes (blue arrows) thus confirming the diagnosis of epidermal inclusion cyst.
DISCUSSION
Manual SICS is the most common surgery performed in developing countries. The incidence of conjunctival cyst is more with SICS than with phacoemulsification as per literature.
We report two cases of SICS with post-operative conjunctival inclusion cysts. In both the cases superior tunnel was made. Hence, cases presented with superior conjunctival cysts. A conjunctival cyst closely resembles a filtering bleb which forms the most common differential diagnosis. In trabeculectomy, a filtering bleb is an intentionally created passage for aqueous to the sub-conjunctival space but it may be unintentionally created following conventional manual SICS. The previous authors reporting conjunctival cysts post SICS have reported fish mouthing of the internal opening on gonioscopic evaluation.[11] This behaves like an unplanned filtering bleb. Visual assessment, intraocular pressure, and external leakage are important indicators to make the decision to intervene. Leaking bleb and over filtration, bleb may result in a decrease in vision due to maculopathy secondary to hypotony and rarely endophthalmitis and spontaneous rupture.
In our cases, both the blebs were encysted within the scleral tunnel but not communicating with the anterior chamber, the decision to intervene was taken despite normal IOP and negative seidels in view of tunnel fish-mouthing and compromised tunnel architecture.
Although the exact mechanisms remain unclear, it is believed that the cysts arise due to the proliferation and accumulation of conjunctival epithelium within the trapped tissue. Surgical trauma during surgery can disrupt the normal anatomy of the conjunctiva, leading to the entrapment of the conjunctiva within the scleral tunnel. Both our cases were resident surgeries with the possibility of excessive cautery, poor tunnel architecture, and improper conjunctival approximation at the end of surgery as probable reasons for conjunctival inclusion cysts. Conjunctival inclusion cysts typically do not cause significant symptoms but may present with mild foreign body sensations or cosmetic issues. While some cysts may resolve on their own, persistent cases or those freely communicating with the anterior chamber necessitates treatment. Surgical excision is considered the optimal approach, and alternative options include thermal cautery under slit-lamp visualisation[12] or YAG laser treatment.[13] Vigilance in post-operative follow-up and prompt management of any cystic formations is crucial to prevent potential complications and ensure optimal patient outcomes. In our cases, the diagnostic dilemma was whether to take up the patient for surgical management or not. Finally, the decision to do surgical excision with suturing of the scleral tunnel was made. The approach involved surgical excision of the cysts followed by watertight closure of the tunnel with sutures. This approach helps eliminate the cysts and reduce the risk of complications like endophthalmitis. From our cases, we note that conjunctival inclusion cysts can occur following uneventful manual SICS.
CONCLUSION
Scleral wound closure is an important step to minimise this complication, if the scleral wound is found to be unstable, it should always be sutured. Excessive conjunctival dissection and excessive cautery which results in leaky tunnels should be avoided. We must also avoid repeated inclusion of conjunctiva through the tunnel during surgery.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Conflicts of interest
There are no conflicts of interest.
Use of artificial intelligence (AI)-assisted technology for manuscript preparation
The authors confirm that there was no use of artificial intelligence (AI)- assisted technology for assisting in the writing or editing of the manuscript and no images were manipulated using AI.
Financial support and sponsorship
Nil.
References
- Conjunctival inclusion cyst presenting as proptosis: A rare scenario. Kerala J Ophthalmol. 2021;33:78-80.
- [CrossRef] [Google Scholar]
- Giant secondary conjunctival inclusion cysts: A late complication of strabismus surgery. Ophthalmology. 2006;113:1049.e1-2.
- [CrossRef] [PubMed] [Google Scholar]
- Conjunctival inclusion cyst following pars plana vitrectomy. Arch Ophthalmol. 2003;121:1067.
- [CrossRef] [PubMed] [Google Scholar]
- Massive epithelium-lined inclusion cysts after scleral buckling. Am J Ophthalmol. 1992;113:439-42.
- [CrossRef] [PubMed] [Google Scholar]
- Large conjunctival inclusion cyst after anterior approach ptosis surgery. Middle East Afr J Ophthalmol. 2022;29:163-6.
- [CrossRef] [PubMed] [Google Scholar]
- Massive iatrogenic orbital cysts following glaucoma drainage implant and strabismus surgery. BMJ Case Rep. 2016;2016:bcr2016216486.
- [CrossRef] [PubMed] [Google Scholar]
- Inadvertent filtering bleb following sutureless cataract surgery. Indian J Ophthalmol. 2005;53:196-8.
- [CrossRef] [PubMed] [Google Scholar]
- Conjunctival inclusion cysts following small incision cataract surgery. Indian J Ophthalmol. 2010;58:423-5.
- [CrossRef] [PubMed] [Google Scholar]
- Postoperative conjunctival cyst: A masquerade. Indian J Ophthalmol. 2011;59:406-7.
- [CrossRef] [PubMed] [Google Scholar]
- Unintentional filtration following cataract surgery. Arch Ophthalmol. 1964;71:43-9.
- [CrossRef] [PubMed] [Google Scholar]
- Tenon's cyst presenting as a long-term complication following incision cataract surgery. Case Rep Med. 2013;2013:759267.
- [CrossRef] [PubMed] [Google Scholar]
- Thermal cautery as a treatment for conjunctival inclusion cyst after strabismus surgery. J AAPOS. 2001;5:48-9.
- [CrossRef] [PubMed] [Google Scholar]
- Treatment of acquired inclusion cyst of conjunctiva using YAG laser. Am J Ophthalmol. 1984;98:807-8.
- [CrossRef] [PubMed] [Google Scholar]







