Translate this page into:
Study of ocular manifestations of COVID-19 patients in a tertiary care hospital of Rural North Maharashtra
*Corresponding author: Ketaki Bhat, Department of Ophthalmology, JMF’S ACPM Medical College, Dhule, Maharashtra, India. doctorketaki@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Bhat K, Wadgaonkar S, More S, Patil G, Heda AS. Study of ocular manifestations of COVID-19 patients in a tertiary care hospital of Rural North Maharashtra. Glob J Cataract Surg Res Ophthalmol. 2023;2:54-8. doi: 10.25259/GJCSRO_16_2023
Abstract
Objectives:
The purpose of the study is to understand profile of ocular manifestations in recovered post COVID 19 patients and to suggest recommendations based on observations.
Materials and Methods:
It was a prospective hospital-based case analysis study done at tertiary care hospital of rural North Maharashtra from April 2020 to June2021 and included 104 patients with recent history of COVID 19 infection and various ocular symptom
Results:
Diabetes mellitus is most common associated factor observed. Viral conjunctivitis was observed in 52 cases .2 cases reported subconjunctival hemorrhage. Retinal vein occlusions were seen in 3 cases. Total ophthalmoplegia was seen in 23 cases. Orbital cellulitis with mucormycosis was documented in 12 cases. Orbital apex syndrome with an impending intracranial spread in 4 case required orbital exenteration. Peribulbar Amphotericin B was given in 3 cases and intravenous and oral antifungals also given simultaneously
Conclusion:
COVID 19 infection can lead to various ocular symptoms even in the recovery period. Early diagnosis by high degree of suspicion and prompt treatment with multidisciplinary approach is required for prevention of visual disability.
Keywords
Orbital cellulitis
COVID19 and Eye
Allergic conjunctivitis
Mucormycosis
INTRODUCTION
COVID-19 is a novel disease that has caused a pandemic, unlike any other disease which we have experienced in modern medicine, not only because of the characteristics of the disease but also due to the rapidity of the spread of infection.
Some recent studies have shown that this new coronavirus strain can lead to conjunctival findings and can be detected in tears and conjunctival secretions.[1] SARS-CoV-2 RNA has been detected through a reverse transcription–polymerase chain reaction (PCR) on conjunctival samples in 0–15% of infected patients.[2,3]
The prevalence of eyelid, ocular surface, and anterior segment manifestations in different studies has varied from 0.81% to 34.5%.[4,5] In COVID-19-recovered patients, a wide range of ocular symptoms is noted. Conjunctivitis is the most common manifestation and can develop at any stage of the disease. The exact pathogenetic mechanisms of the conjunctival infection are still unknown.[6]
The present study aimed to study the profile of different ocular manifestations in recovered post-COVID-19 patients in tertiary care hospitals.
MATERIALS AND METHODS
The present study was a single-centre, prospective study conducted in the department of ophthalmology of a tertiary care hospital in rural North Maharashtra. The institutional ethics committee approved the study.
Our study is a prospective hospital-based case analysis study with a total of 104 cases. This was done for 14 months starting from April 2020 to June 2021.
Inclusion criteria
The following criteria were included in the study:
All patients recovered from COVID-19 infection (confirmed with PCR with nasopharyngeal swab samples) having ocular symptoms
We included patients within 3 months of COVID-19 infection
Adult patients with age ≥18 years
Patients who gave consent for participation in the study.
Data collected included demographic details as well as any medical or surgical comorbidities and ongoing treatment. A thorough ophthalmic examination was done in each case who came to the eye outpatient department (OPD) including visual acuity with Snellen’s chart. We did Schirmer’s test without anaesthetics in suspected cases of dry eyes. We noted pupillary reaction and a detailed slit lamp examination was done. Fundus examination with the help of a 90D lens and indirect ophthalmoscopy was done. We measured intraocular pressure with Goldman’s applanation tonometer/non-contact tonometer wherever possible. Patients who were admitted to the intensive care unit or ward setup were examined with the help of torchlight and direct ophthalmoscopy as per feasibility. Later these patients were evaluated in detail in eye OPD once they were discharged. We also recorded computed tomography scans of the brain, paranasal sinus, and orbit findings in cases wherever it was needed.
We noted the treatment history of injection remdesivir and injection dexamethasone from patients by reviewing the discharge summary. Statistical analysis was done using descriptive statistics.
RESULTS
In the present study, 104 patients were included. The majority of patients were from the young age group of 35–50 years and males (n = 69) outnumbered females (n = 35). Table 1 shows distribution of cases based on epidemiological profile and treatment received.
| Characteristics | No. of patients (n=104) | Percentages |
|---|---|---|
| Age distribution | ||
| 20–35 years | 34 | 32.7 |
| 35–50 years | 46 | 44.2 |
| >50 years | 24 | 23.1 |
| Gender | ||
| Male | 69 | 66.3 |
| Female | 35 | 33.7 |
| Comorbidities | ||
| Diabetes mellitus | 47 | 45.19 |
| Hypertension | 16 | 15.4 |
| History of chronic ocular disease | 12 | 11.5 |
| Period since COVID-19 infection | ||
| <1 month | 69 | 66.3 |
| 1–3 months | 21 | 20.2 |
| >3 months | 14 | 13.5 |
| Treatment received | ||
| Injection Remdesivir | 69 | 66.3 |
| Injection Dexamethasone | 69 | 66.3 |
| Required ventilation | 46 | 44.2 |
| Non-invasive | 19 | 18.3 |
| Invasive | 25 | 24.0 |
Diabetes mellitus (DM) (45.19%) was the most common comorbidity noted in study patients. The majority of patients presented with ocular symptoms in <1 month following COVID-19 infection (66.3%). For treatment of COVID-19 infection, the main medications received by study patients were injection remdesivir (66.3%) and injection dexamethasone (66.3%). Out of 104 cases under study, 46 (44.2%) patients required ventilator support during the treatment period.
In our study, we observed dryness of the eyes as the most common symptom in 31 cases (29.8%). Diagnosis of dry eye was confirmed with Schirmer’s test. Table 2 distribution of patients based on symptoms and signs observed.
| Symptoms | Number of patients (n=104) | Percentages % |
|---|---|---|
| Dryness of eyes | 31 | 29.8 |
| Pain | 19 | 18.3 |
| Discharge | 17 | 16.3 |
| Redness | 14 | 13.5 |
| Watering | 11 | 10.6 |
| Foreign body sensation | 9 | 8.7 |
| Burning sensation | 9 | 8.7 |
| Photophobia | 8 | 7.7 |
| Blurred vision | 7 | 6.74 |
| Itching in eyes | 6 | 5.8 |
| Signs | Number of patients (n=104) | Percentages % |
| Chemosis | 3 | 2.9 |
| Lid margin hyperemia | 29 | 27.9 |
| Crusted eyelashes | 25 | 24.0 |
| Meibomian abnormality | 14 | 13.5 |
| Follicular conjunctivitis | 8 | 7.7 |
In our study, the most common anterior segment pathology was observed viral conjunctivitis (47.11%), followed by orbital cellulitis with mucormycosis (20.19%). Table 3 shows cases distribution based on clinical diagnosis.
| Diagnosis | No. of patients (n=104) | Percentages % |
|---|---|---|
| Viral conjunctivitis | 49 | 47.11 |
| Orbital cellulitis with mucormycosis | 21 | 20.19 |
| Partial third nerve palsy | 14 | 13.5 |
| Total ophthalmoplegia with no PL | 13 | 12.5 |
| Orbital apex syndrome with impending intracranial spread |
5 | 4.80 |
| Subconjunctival haemorrhage | 3 | 2.88 |
| Retinal vein occlusion | 3 | 2.9 |
PL: Perception of light
Orbital cellulitis is a severe and vision-threatening complication seen in COVID patients. An aggressive multidisciplinary approach is required for salvaging vision. Cellulitis with mucormycosis was observed in 21 patients (20.19%), majority of them were male (71.42%). Figure 1 shows case of orbital mucormycosis treated with surgical debridement. Injection amphotericin B (peribulbar, 3.5 mg on alternate days for 3 days) was used in 12 patients (57.14%) and oral posaconazole was used in 16 patients (76.19%). Surgical debridement was required in 12 patients (57.14%) and two patients required orbital exenteration. Mucormycosis cases were consulted by ENT and Dental specialists for combined management. Table 4 shows characteristics of patients presented with ocular mucormycosis. Partial 3rd nerve palsy with intact extra ocular movements was seen 14 cases. (13.5%) Figure 2 shows case of Partial 3rd nerve palsy.
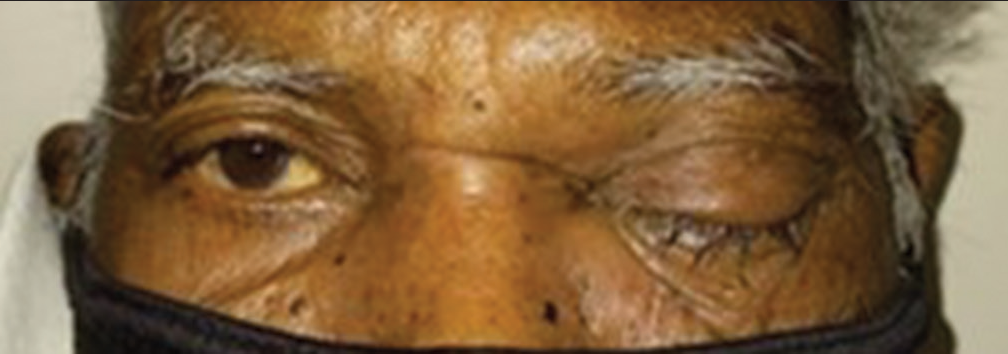
- Post COVID19 Orbital Cellulitis treated with surgical debridement.
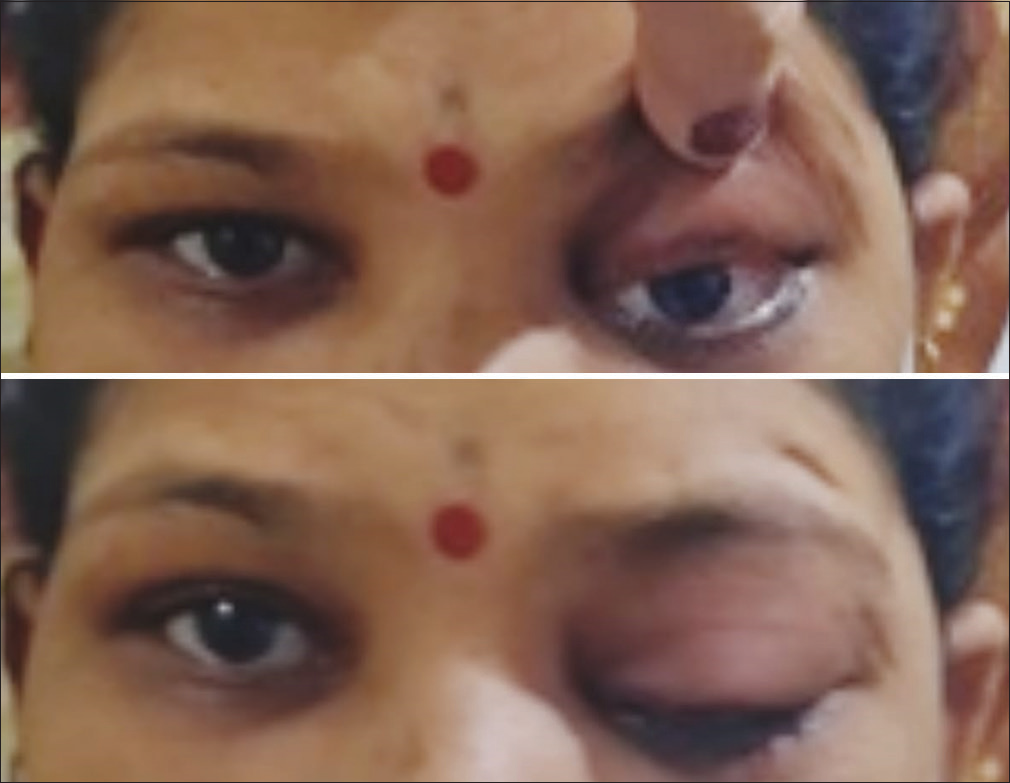
- Partial 3rd nerve palsy in Left eye with intact extra ocular movements.
| Characteristic | No. of patients | Percentages % |
|---|---|---|
| Orbital cellulitis with mucormycosis | 21 | 20.19 |
| Gender | ||
| Male | 15 | 71.44 |
| Female | 6 | 28.56 |
| Treatment | ||
| Surgical debridement | 12 | 57.14 |
| Peribulbar | 12 | 57.14 |
| Oral posaconazole | 16 | 76.19 |
| Orbital exenteration | 2 | 9.5 |
DISCUSSION
Signs of COVID-19 conjunctivitis are similar to those of other viral infections, mostly bilateral conjunctival hyperemia, chemosis, the follicular reaction of the tarsal conjunctiva, epiphora, watery discharge, mild eyelid oedema, and enlarged preauricular and submaxillary lymph nodes.[7] Direct effects due to the virus, immune-mediated tissue damage, activation of the coagulation cascade, and prothrombotic state induced by the viral infection and drugs used in the management are proposed mechanisms for conjunctival infection.[6]
A review and meta-analysis of 16 studies was done by Aggarwa et al.[8] included 2347 patients and a prevalence of 11.6% was observed.
Conjunctivitis is the most common ophthalmic manifestation documented in COVID-19 patients by Sindhuja et al.[4] They reported that 8.66% of patients had conjunctivitis in cases with mild COVID-19 infection. In a study from Wuhan, China, from a total of 535 patients, about 20% had dry eye, 12% had blurred vision, 11% had foreign body sensation, 10% had epiphora and 9% had increased ocular secretion.[9]
Two meta-analyses reported that conjunctivitis presented in 1.1% of COVID-19 patients[10] and the pooled prevalence of conjunctivitis among COVID-19 patients was 5.5%.[11]
Sen et al.[6] studied 120 patients with ocular surface symptoms following COVID-19. The mean age was 45 years.
Tyagi et al.[12] noted that from 1950 patients, only 7 (0.36%) had ophthalmic manifestations with conjunctival congestion being the most common sign (42.8%) observed. Similar findings were noted in the present study where viral conjunctivitis (47.11%) was the most commonly observed ocular manifestation.
Chen et al.[5] found that 27 (5.04%) out of the 535 patients with COVID-19 had conjunctival congestion and the average duration of conjunctival congestion was 4.5 days.
Conjunctivitis (6.2%), xerophthalmia (4.5%), and keratitis (2.6%) were noted among them. Frequent hand-to-eye contact may be a risk factor for conjunctival congestion in patients with COVID-19.
There was a high frequency of ocular manifestations in hospitalized COVID patients and probably ocular manifestations could be a sign of more severe COVID disease. It could be a presenting sign of COVID and this should be kept in mind in all patients presenting with ocular manifestations, red eye in particular.[13]
The use of steroids, monoclonal antibodies, and broad-spectrum antibiotics for the management of COVID-19 illness can increase the chances of new-onset fungal infection or exacerbate a pre-existing one.[14]
The suggested mechanism for post-COVID orbital cellulitis and sinusitis is COVID-19-induced upper respiratory congestion which can compromise mucociliary clearance. Mucormycosis is an angioinvasive disease caused by fungi Mucorales such as Rhizopus, Mucor, Rhizomucor, Cunninghamella, and Absidia. The prevalence of mucormycosis in India is approximately 0.14 cases/1000 population, about 80 times the prevalence in developed countries.[15]
Morbidity and mortality due to mucormycosis vary depending on the underlying medical condition, fungus type, and location. Mucormycosis is one of the serious, opportunistic infections noted in moderate-to-severe COVID-19. Compromised immune system with decreased CD4+ and CD8+ lymphocytes with associated comorbidities (e.g., DM and chronic obstructive pulmonary disease) and immunocompromised conditions (e.g., corticosteroid therapy, ventilation, and intensive care unit stay) were major factors for mucormycosis in COVID-19 patients.[16]
Diagnosis of mucormycosis remains challenging. The clinical approach helps in raising suspicion and prompting the initiation of laboratory testing. Histopathology, direct examination, and culture remain essential tools. John et al.[17] conducted a review of 41 cases of COVID-19-associated mucormycosis (CAMCR) and noted that CAMCR was typically seen in patients with DM (94%), especially the ones with poorly controlled DM (67%) and severe or critical COVID-19 (95%). DM is a significant risk factor for secondary infections.
Conservative debridement and transcutaneous retrobulbar injection of amphotericin B are being increasingly considered reasonable first-line options.[18] Even with rapid diagnosis and initiation of treatment, prognosis is poor with mortality ranging from 21% to 80%.[19,20]
Steroids and immunosuppressive medications must be used with caution during therapy, particularly in aged, immunocompromised, cancer, and diabetic patients with COVID.[21] A high index of suspicion, early diagnosis with histopathological and microbiological evidence, appropriate management with antifungals and aggressive surgical debridement (functional endoscopic sinus surgery and orbital exenteration) can improve survival in patients of mucormycosis in COVID-19 patients.
CONCLUSION
COVID-19 can lead to various ocular symptoms even in the recovery period. It can lead to severe diseases such as mucormycosis. Early diagnosis with a high degree of suspicion and prompt treatment with a multidisciplinary approach is required for the prevention of visual disability.
Limitations of the study
As COVID-19 is a novel disease with varied presentations, many symptoms and signs are overlapping. We could not pinpoint the exact recovery period from the disease itself. Other factors such as the effect of the vaccine, treatment response to various therapies, and virulence of the virus strain may have affected ocular findings. Long-term sequelae could not be evaluated as many patients were lost to follow-up in the ophthalmology department.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Conflicts of interest
Dr. Aarti Subhash Heda is on the editorial board of the Journal.
Use of artificial intelligence (AI)-assisted technology for manuscript preparation
The author(s) confirms that there was no use of artificial intelligence (AI)-assisted technology for assisting in the writing or editing of the manuscript and no images were manipulated using AI.
Financial support and sponsorship
Nil.
References
- Evaluation of Coronavirus in tears and conjunctival secretions of patients with SARS-CoV-2 infection. J Med Virol. 2020;92:589-94.
- [CrossRef] [PubMed] [Google Scholar]
- COVID-19 disease and ophthalmology: An update. Ophthalmol Ther. 2020;9:1-12.
- [CrossRef] [PubMed] [Google Scholar]
- COVID-19 and the eye: How much do we really know? A best evidence review. Arq Bras Oftalmol. 2020;83:250-61.
- [Google Scholar]
- Clinical profile and prevalence of conjunctivitis in mild COVID-19 patients in a tertiary care COVID-19 hospital: A retrospective cross-sectional study. Indian J Ophthalmol. 2020;68:1546-50.
- [CrossRef] [PubMed] [Google Scholar]
- Ocular manifestations and clinical characteristics of 535 cases of COVID-19 in Wuhan, China: A cross-sectional study. Acta Ophthalmol. 2020;98:e951-9.
- [CrossRef] [Google Scholar]
- COVID-19 and eye: A review of ophthalmic manifestations of COVID-19. Indian J Ophthalmol. 2021;69:488-509.
- [CrossRef] [PubMed] [Google Scholar]
- Ocular findings in Covid-19 patients: A review of direct manifestations and indirect effects on the eye. J Ophthalmol. 2020;2020:4827304.
- [CrossRef] [PubMed] [Google Scholar]
- Ocular surface manifestations of Coronavirus disease 2019 (COVID-19): A systematic review and meta-analysis. PLoS One. 2020;15:e0241661.
- [CrossRef] [PubMed] [Google Scholar]
- The ocular surface, Coronaviruses and COVID-19. Clin Exp Optom. 2020;103:418-24.
- [CrossRef] [PubMed] [Google Scholar]
- Conjunctivitis and COVID-19: A meta-analysis. J Med Virol. 2020;92:1413-4.
- [CrossRef] [PubMed] [Google Scholar]
- The prevalence of ophthalmic manifestations in COVID-19 and the diagnostic value of ocular tissue/fluid. Graefes Arch Clin Exp Ophthalmol. 2020;258:1351-2.
- [CrossRef] [PubMed] [Google Scholar]
- Ocular manifestations in Covid-19 positive patients admitted to a tertiary care centre in Uttarakhand, India: A prospective study. Int J Health Clin Res. 2021;4:225-8.
- [Google Scholar]
- Ocular manifestations of hospitalized patients with COVID-19 in Northeast of Iran. Ocul Immunol Inflamm. 2020;28:739-44.
- [CrossRef] [PubMed] [Google Scholar]
- Rhino-orbital mucormycosis associated with COVID-19. Cureus. 2020;12:e10726.
- [CrossRef] [Google Scholar]
- Epidemiology and diagnosis of mucormycosis: An update. J Fungi (Basel). 2020;6:265.
- [CrossRef] [PubMed] [Google Scholar]
- COVID-19 and orbital mucormycosis. Indian J Ophthalmol. 2021;69:1002-4.
- [CrossRef] [PubMed] [Google Scholar]
- When uncontrolled diabetes mellitus and severe COVID-19 converge: The perfect storm for mucormycosis. J Fungi (Basel). 2021;7:298.
- [CrossRef] [PubMed] [Google Scholar]
- Invasive fungal sinusitis: Treatment of the orbit. Curr Opin Ophthalmol. 2017;28:522-33.
- [CrossRef] [PubMed] [Google Scholar]
- Orbital and cranial nerve presentations and sequelae are hallmarks of invasive fungal sinusitis caused by Mucor in contrast to Aspergillus. Am J Rhinol. 2008;22:155-8.
- [CrossRef] [PubMed] [Google Scholar]
- Invasive fungal disease of the sinus and orbit: A comparison between mucormycosis and Aspergillus. Br J Ophthalmol. 2016;100:184-8.
- [CrossRef] [PubMed] [Google Scholar]
- A contemporary intimidation for COVID-19 patients coinfected with mucormycosis in India. J Bacteriol Mycol Open Access. 2021;9:69-71.
- [CrossRef] [Google Scholar]







